The shoulder is the most flexible joint in your body that helps you to rotate your arm in many positions – upward, to the side, in front, and behind. However, this flexibility also increases the susceptibility of the shoulder joint to instability and injuries.
For Shoulder joint pathologies, non-surgical treatment options may be recommended, however, in certain conditions, Surgery is the choice of treatment as delaying the surgery can increase the likelihood of more serious problems. An early diagnosis and treatment of the joint can help make a significant difference in the quality of life and function in the long run.

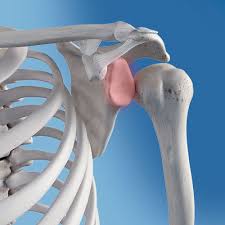
- Bursitis or Tendinitis – Bursitis refers to inflammation of the bursa, a fluid-filled sac acting as a cushion between bone and other moving parts like tendons, skin, or muscles. Tendinitis, on the other hand, is the inflammation of the tendon. Bursitis and Tendinitis occur due to overactivity of the joint or because of repetitive activities like swimming, painting, etc. These repetitive activities lead to squeezing and rubbing off the rotator cuff (a group of muscles and tendons attaching your upper arm to the shoulder blade). Initially, the condition may be treated by activity modification for pain alleviation and shoulder rehabilitation. However, in complicated cases, surgery may be advised.
- Impingement & Partial Rotator Cuff Tears – The condition may be associated with chronic inflammation and spur formation on the underside of the Acromion or Acromioclavicular joint. The conservative treatment involves activity modification, cortisone injection, and light exercises. If the conservative treatment fails to relieve pain and symptoms, surgery is advised for the removal of spurs from the underside of the acromion, and the rotator cuff is repaired.
- Full Thickness Rotator Cuff Tears – Full Thickness Rotator Cuff tears happen due to partial thickness rotator cuff tears, falls, heavy weight lifting, and impingement. If non-surgical treatment for pain relief such as activity modification remains unsuccessful, surgery for the full-thickness rotator cuff tear may be required. To an extent, Arthroscopic techniques help in the shaving of spurs and, the evaluation and repair of rotator cuff tears. And, both techniques require extensive rehabilitation for the restoration of shoulder joint function.
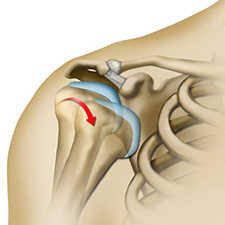
- Shoulder Instability – Shoulder Instability occurs when the head of the upper arm is forced out of the shoulder socket owing to sudden injury or overuse of the shoulder ligament. The two types of dislocation are subluxation and dislocation. Subluxation means partial or incomplete dislocation whereas dislocation refers to the condition when the shoulder completely moves out of the shoulder joint. If subluxation remains untreated, it eventually gets dislocated. Patients who have recurrent shoulder dislocations usually require surgery. Open surgery is usually the preferred choice for treatment and requires a short hospital stay & arthroscopic surgery can be done on an outpatient basis.
- Fractured Collarbone & Acromioclavicular Joint – Fractures of the collarbone and acromioclavicular joint usually occur in children upon falling on the side of their shoulders while playing. Severe dislocations may require surgical repair also.
- Fractured Head of Humerus – Falling on an outstretched arm can lead to a fracture of the humerus (arm bone). It usually happens in older people with osteoporosis. If completely fragmented or displaced, a fracture of the shoulder joint may require an open surgical repair, and in complicated cases, it may require a prosthesis.
- Osteoarthritis & Rheumatoid Arthritis – Degenerative arthritis like osteoarthritis of the shoulder joint can lead to joint degeneration, and tearing of the capsule or rotator cuff. Rheumatoid arthritis of the shoulder joint involves synovial inflammation and such conditions may require surgery.
At CSI, we plan for a comprehensive Orthopaedic Evaluation which involves three main components:
- Patient’s Medical History – The patient’s medical history is gathered to collect information about pain, injury, symptoms, and limitations. It also helps the doctors with the past medical/surgical history of the patient.
- Physical Examination – This helps the doctor with the assessment of swelling, tenderness, joint range of motion, muscle strength, weakness, instability, or deformity of the shoulder.
- Diagnostic Tests – Tests like X-ray, MRI, and CT for assessing the bony and soft tissue parts help with making an accurate diagnosis. CSI has a dedicated Imaging Center, DiagKnow that helps our doctors make an accurate diagnosis of sports/orthopedic injury and helps them with an informed decision about whether the person needs surgery or conservative treatment.
Types of Surgery – Orthopaedic surgery can be Arthroscopic or an Open Surgery
- Arthroscopy – It is a procedure that involves the orthopedic surgeon inserting a pencil-thin device with a small lens and lighting system into a tiny incision in the joint. The images are relayed on a TV screen and help make an accurate diagnosis of the patient’s condition. The procedure may also involve inserting other surgical instruments to make repairs with the help of an arthroscope. Arthroscopy is usually done on an outpatient basis.
- Open Surgery – Open surgery is a surgical procedure done by making small incisions of a few inches and performing the surgery on the exposed structure. It can have a better outcome than arthroscopy.
Recovery and rehabilitation depend upon the type of surgery performed on the shoulder irrespective of whether it was arthroscopic or open surgery.
The patient is advised to be Nil By Mouth before surgery. They are advised not to eat or drink anything after midnight before surgery. Discuss with your surgeon about the medication to be consumed during the morning. The patient undergoes a Pre-anaesthetic check-up before surgery to know about being favorable to undergo anesthesia during surgery.
How do I prepare for the surgery?
Within a month of the surgery, the following things must be ascertained about you:
- Get a complete orthopedic evaluation done at CSI by making an appointment with the orthopedic doctor at CSI
- You will undergo a complete history and physical examination
- You will be advised for various tests like CBC and electrocardiogram, all being available at CSI and then you will be advised for the advanced meeting and counseling about the procedure with the doctor.
The day before the surgery, you will be advised to stay at NBM and wash the area several times to decrease the risk of infection. In case you have to have medication in the morning, you should consult your doctor about them.
What type of anesthetic will I be given during the surgery?
This completely depends upon the surgery you are undergoing. You can be given General anesthesia that will make you sleep during the entire procedure or you can remain awake after you get local anesthesia for your surgery.
How is arthroscopy done?
Although easier than open surgery, Arthroscopy still requires the use of anesthetics and you will be given either general or local anesthesia, as per the discretion of the surgeon. Earlier, arthroscopy was used as a diagnostic tool only but with the development of technology, it is used as a surgical procedure also.
What conditions are treated with a combination of Arthroscopy & Standard Surgery?
Combining arthroscopy with standard surgery can treat several conditions such as:
- Rotator Cuff Repair
- Bankart Repair
- Capsular Shift
- Removal of inflamed synovium (lining) of shoulder
- Repair/resection of torn ligament of the shoulder joint
- Repair of torn ligament
How is a torn rotator cuff surgically repaired?
Most of the rotator cuffs are surgically repaired by the reattachment of the torn tendons of the humerus. This is done by both arthroscopically and by open surgery. Suturing is done on the torn tendons. The tendons heal back with time and the tendon-to-bone connection is secured. It takes weeks to months for the tendon to heal back to the bone.
What are the possible complications after surgery?
Common complications during surgery can be Infection, phlebitis, excessive bleeding, swelling, joint stiffness, etc. However, at CSI, you are ably taken care of before any serious complications arise. Trust us, you are at the right place and under the caring hands.
What is the possible recovery time post Shoulder Surgery?
The arthroscopic punctures may take several days to heal. Although the operative dressing is removed the morning after the day of the surgery, and adhesive strips are applied to cover the small incisions, it may take several weeks (6-8 weeks) for the joint to get fully repaired. Precautions must be taken and specific activities must be restricted, as advised by the surgeon.
- Rehabilitation
- Non-Surgical
- Post- Surgical
- PRP
CSI is a one-stop solution for the treatment and management of all sorts of orthopedic, musculoskeletal, and sports-related injuries. Right from the evaluation of the condition to assessments through imaging techniques to surgery and post-operative rehabilitation, CSI is the ultimate solution for all your orthopedic conditions.
CSI is one of the best orthopedic hospitals in South Delhi, India, run under the leadership of the best orthopedic and sports surgeon in Delhi – Dr. Pushpinder Singh Bajaj.
Page Under Construction!
